 Pharma & Payers
Pharma & Payers
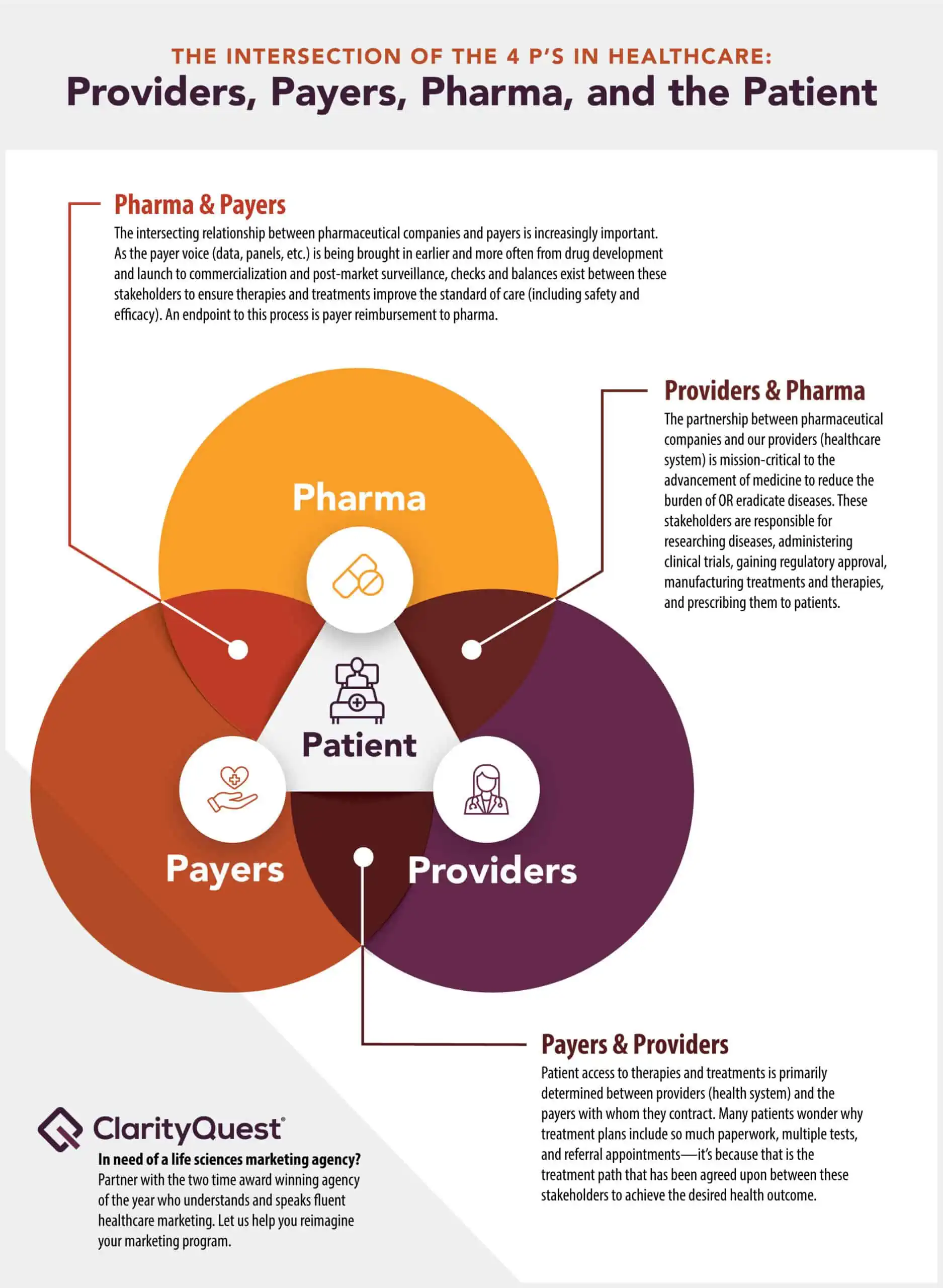
The intersecting relationship between pharmaceutical companies and payers is increasingly important. As the payer voice (data, panels, etc.) is being brought in earlier and more often from drug development and launch to commercialization and post-market surveillance, checks and balances exist between these stakeholders to ensure therapies and treatments improve the standard of care (including safety and efficacy). An endpoint to this process is payer reimbursement.
Providers & Pharma
The partnership between pharmaceutical companies and our providers (healthcare system) is mission-critical to the advancement of medicine to reduce the burden of OR eradicate diseases. These stakeholders are responsible for researching diseases, administering clinical trials, gaining regulatory approval, manufacturing treatments and therapies, and prescribing them to patients.
Payers & Providers
Patient access to therapies and treatments is primarily determined between providers (health system) and the payers with whom they contract. Many patients wonder why treatment plans include so much paperwork, multiple tests, and referral appointments—it’s because that is the treatment path that has been agreed upon between these stakeholders to achieve the desired health outcome.
In need of a life sciences marketing agency? Partner with the two-time award-winning agency of the year that understands and speaks fluent healthcare marketing.
Let us help you reimagine your marketing program.
 Pharma & Payers
Pharma & Payers